Andrew Haldenby is co-founder of Aiming for Health Success, a new health research body, alongside Professor Nick Bosanquet.
The NHS exits the pandemic with not only a backlog of two million hospital patients, but also the longest waiting times for 30 years.
300,000 people are waiting for hospital treatment for 12 months or more on the latest figures, compared to just 1,500 in January 2020. As a proportion of the waiting list, year-long waits are now at the same level as in 1992. Waiting times are a measure of suffering because many conditions worsen over time. The hospital backlog is a historic threat to patient care and wellbeing.
The NHS has offered varying responses. The NHS Confederation, representing hospitals and other providers, asked the Prime Minister in February to be “honest” and to tell the public to expect year-long waits “for some years”. Against that, I have spoken to hospital leaders who are doing all they can to tackle waiting lists, including running operating theatres until midnight and considering a 24-hour service.
Ministers should be firmly on the side on the side of the latter group. There is no reason for the current situation to become a new normal. Matthew Hancock and colleagues should expect the NHS to eliminate the backlog in full before the next general election.
The solution does not lie in a “bigger” NHS. The Service will not increase hospital bed numbers or workforce for at least the next five years, despite the headline commitments in the 2019 Conservative manifesto.
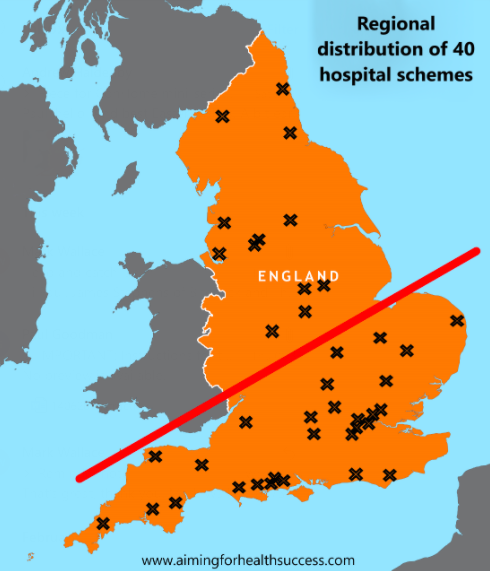
Of the “40 new hospitals” programme, only three have firm finish dates before 2024. (Even after that, the programme is a series of refurbishments rather than new builds. As the map shows, it does not benefit the whole country, with the great majority of projects taking place in London and the South of England).
Ministers recently announced an increase of 10,000 nurses over the last year, fuelled largely by overseas recruitment. Their problem is that the number of qualified nurses leaving the service is likely to be at least 15,000 a year. International recruitment will continue but finding local recruits will be harder due to the time taken to increase numbers of trainers. As a result, the manifesto target of 50,000 nurses will maintain rather than grow the workforce.
The aim is not “bigger” but “better” i.e. the sharpest focus on a high-productivity NHS of any government in the Service’s history. The current NHS strategy (laid down in the “ten year plan” in 2019) is good but it wasn’t designed to tackle the current backlog. Ministers need that plan to happen much more quickly and key new policies to come in alongside.
The first goal is to generate the extra activity needed to tackle the backlog. Traditional hospitals, even working extra hours, cannot do this. The new 42 NHS regions (“Integrated Care Systems”) need to establish new high-volume centres on the model of the South West London Elective Orthopaedic Centre (SWLEOC). Opened in 2004, it performs around 5,200 procedures a year. As such it is the largest hip and knee replacement centre in the UK and one of the largest in Europe.
Given the need for new capital to start these centres, the NHS should call on all national and global resources. Some of the centres could be joint ventures with experienced providers such as the Cleveland Clinic and Apollo Healthcare in India. Ministers should expect to see plans for an initial group of 10 centres before the end of the summer, with the first patients being treated next year.
The second goal is the shift towards the new model of care that successive governments have described for the last 15 years. The idea is right: a reorientation of the NHS so that hospitals are no longer the centre of gravity of the Service.
Community services will provide much faster diagnostic scans, often working in partnership with private firms. Strengthened GPs, working with consultants, will lead patients’ treatments, reducing the bottleneck of waiting for hospital appointments. GPs can also work with patients to change their lifestyles, in a way that hospitals cannot. The pandemic has highlighted the problem of obesity which is a key risk factor for long term conditions.
Simon Stevens, the excellent chief executive of the NHS, said last week that “prevention and integration are the holy grail”. His commitment to a more productive NHS is not in doubt but he will know that progress has been difficult. As the NAO has shown, the share of the NHS budget going to hospitals has actually increased in recent years. Both he and Ministers should give local NHS leaders the tools, and the support, to move faster.
On staffing, the focus should be community teams. The current recruitment of 20,000 new staff in primary care networks should be just the beginning of a strengthening of local capacity. As well as adding new entry-level staff, the NHS should support experienced leaders. A special grade of NHS Team Leader, with access to digital learning, mentoring and higher pay, would help.
On funding, reducing the number of hospital outpatient appointments by 30 per cent, as the NHS is committed to do, would release £7 billion per year for new services. Ministers should go further and expect hospitals to reduce inpatient and emergency attendees by a third as well, in this Parliament, helping to turn hospitals into hubs for community services.
Ministers will come under intense pressure to increase NHS spending further in the spending review this autumn. They should resist. Health spending has already risen by a third as a share of GDP (10 per cent now compared 6.9 per cent in 1997). Unless this rise is constrained, it is difficult to see how any government can make progress in other areas. That includes education which is at the heart of any effective levelling-up effort.
On social care, successive Governments have become bogged down in the search for a perfect funding system. In the meantime, social care delivers higher quality care than acute hospitals and is providing welcome new options for care in people’s homes, even for those with complex needs. Ministers may not need a grand plan. Simply providing realistic funding for local-authority financed care residents would provide security for operators. The worst approach would be to nationalize social care as a free service under the NHS, leading to higher costs and much worse access.
Last week Sir David Nicholson, the previous head of the NHS, said that waiting times could reach two years by the next election. The Guardian reported that lengthening delays for treatment will be a “major political problem” for Boris Johnson. This need not be the case. After the success of the vaccine programme, tackling the backlog could be the Government’s lasting achievement.
Andrew Haldenby is co-founder of Aiming for Health Success, a new health research body, alongside Professor Nick Bosanquet.
The NHS exits the pandemic with not only a backlog of two million hospital patients, but also the longest waiting times for 30 years.
300,000 people are waiting for hospital treatment for 12 months or more on the latest figures, compared to just 1,500 in January 2020. As a proportion of the waiting list, year-long waits are now at the same level as in 1992. Waiting times are a measure of suffering because many conditions worsen over time. The hospital backlog is a historic threat to patient care and wellbeing.
The NHS has offered varying responses. The NHS Confederation, representing hospitals and other providers, asked the Prime Minister in February to be “honest” and to tell the public to expect year-long waits “for some years”. Against that, I have spoken to hospital leaders who are doing all they can to tackle waiting lists, including running operating theatres until midnight and considering a 24-hour service.
Ministers should be firmly on the side on the side of the latter group. There is no reason for the current situation to become a new normal. Matthew Hancock and colleagues should expect the NHS to eliminate the backlog in full before the next general election.
The solution does not lie in a “bigger” NHS. The Service will not increase hospital bed numbers or workforce for at least the next five years, despite the headline commitments in the 2019 Conservative manifesto.
Of the “40 new hospitals” programme, only three have firm finish dates before 2024. (Even after that, the programme is a series of refurbishments rather than new builds. As the map shows, it does not benefit the whole country, with the great majority of projects taking place in London and the South of England).
Ministers recently announced an increase of 10,000 nurses over the last year, fuelled largely by overseas recruitment. Their problem is that the number of qualified nurses leaving the service is likely to be at least 15,000 a year. International recruitment will continue but finding local recruits will be harder due to the time taken to increase numbers of trainers. As a result, the manifesto target of 50,000 nurses will maintain rather than grow the workforce.
The aim is not “bigger” but “better” i.e. the sharpest focus on a high-productivity NHS of any government in the Service’s history. The current NHS strategy (laid down in the “ten year plan” in 2019) is good but it wasn’t designed to tackle the current backlog. Ministers need that plan to happen much more quickly and key new policies to come in alongside.
The first goal is to generate the extra activity needed to tackle the backlog. Traditional hospitals, even working extra hours, cannot do this. The new 42 NHS regions (“Integrated Care Systems”) need to establish new high-volume centres on the model of the South West London Elective Orthopaedic Centre (SWLEOC). Opened in 2004, it performs around 5,200 procedures a year. As such it is the largest hip and knee replacement centre in the UK and one of the largest in Europe.
Given the need for new capital to start these centres, the NHS should call on all national and global resources. Some of the centres could be joint ventures with experienced providers such as the Cleveland Clinic and Apollo Healthcare in India. Ministers should expect to see plans for an initial group of 10 centres before the end of the summer, with the first patients being treated next year.
The second goal is the shift towards the new model of care that successive governments have described for the last 15 years. The idea is right: a reorientation of the NHS so that hospitals are no longer the centre of gravity of the Service.
Community services will provide much faster diagnostic scans, often working in partnership with private firms. Strengthened GPs, working with consultants, will lead patients’ treatments, reducing the bottleneck of waiting for hospital appointments. GPs can also work with patients to change their lifestyles, in a way that hospitals cannot. The pandemic has highlighted the problem of obesity which is a key risk factor for long term conditions.
Simon Stevens, the excellent chief executive of the NHS, said last week that “prevention and integration are the holy grail”. His commitment to a more productive NHS is not in doubt but he will know that progress has been difficult. As the NAO has shown, the share of the NHS budget going to hospitals has actually increased in recent years. Both he and Ministers should give local NHS leaders the tools, and the support, to move faster.
On staffing, the focus should be community teams. The current recruitment of 20,000 new staff in primary care networks should be just the beginning of a strengthening of local capacity. As well as adding new entry-level staff, the NHS should support experienced leaders. A special grade of NHS Team Leader, with access to digital learning, mentoring and higher pay, would help.
On funding, reducing the number of hospital outpatient appointments by 30 per cent, as the NHS is committed to do, would release £7 billion per year for new services. Ministers should go further and expect hospitals to reduce inpatient and emergency attendees by a third as well, in this Parliament, helping to turn hospitals into hubs for community services.
Ministers will come under intense pressure to increase NHS spending further in the spending review this autumn. They should resist. Health spending has already risen by a third as a share of GDP (10 per cent now compared 6.9 per cent in 1997). Unless this rise is constrained, it is difficult to see how any government can make progress in other areas. That includes education which is at the heart of any effective levelling-up effort.
On social care, successive Governments have become bogged down in the search for a perfect funding system. In the meantime, social care delivers higher quality care than acute hospitals and is providing welcome new options for care in people’s homes, even for those with complex needs. Ministers may not need a grand plan. Simply providing realistic funding for local-authority financed care residents would provide security for operators. The worst approach would be to nationalize social care as a free service under the NHS, leading to higher costs and much worse access.
Last week Sir David Nicholson, the previous head of the NHS, said that waiting times could reach two years by the next election. The Guardian reported that lengthening delays for treatment will be a “major political problem” for Boris Johnson. This need not be the case. After the success of the vaccine programme, tackling the backlog could be the Government’s lasting achievement.